HR Solutions
Home of the real HR Hero®
HR Hero delivers expert-backed content and ready-to-use resources and workflow tools that save you hours of research and guesswork.
REQUEST A PRODUCT DEMOBuilt for the real work of HR
Policies and handbooks
Build compliant, state-specific employee handbooks and workplace policies with state-specific guidance reviewed and updated by legal experts.
Compensation and job descriptions
Access salary benchmarking data, prewritten job descriptions, and tools that help you ensure equity, compliance, and competitiveness — without starting from scratch.
Compliance guidance and analysis
Stay ahead of shifting federal and state regulations with expert legal analysis, guidance and easy-to-understand explanations of federal and state laws.
Extensive resource library
From onboarding to termination, get step-by-step guidance, Q&As, and how-to articles you can rely on — whether you’re solving a complex issue or training a new manager.
Your hub for all things HR
HR doesn’t stop, and neither do we. With HR Hero, you gain a trusted resource hub that’s continually updated by HR and legal experts, so you can move forward knowing you’re backed by credible, up-to-date information. From legal insights, news, and templates to sample policies, checklists and training modules, HR Hero has you covered.

Confident HR decisions start here
Eliminate expensive hourly consulting rates with the assistance of HR Hero. Our in-house employment law experts are here to help you navigate your most pressing HR questions with the thoroughness you need and the human context you can trust.
Meet the HR toolkit
Accomplish more with integrated solutions that provide access to a team of HR experts, plus actionable templates and workflow resources for writing job descriptions, creating and maintaining a digital employee handbook, accurately classifying employees, and automating risk assessments.
Leave the details to us
With 1,600+ ready-to-use documents, across over 75 employment topics, we provide complete training resources, checklists, forms, and calculators that will allow you to excel in your daily tasks in half the time. Free yourself and your team from administrative burdens so you can focus on strategic initiatives.
HR Solutions
Simplify multi-state compliance with legal analyses, HR training, and best-in-class tools for your team.
BROWSE ALL SOLUTIONSEmployee Handbook Builder
Build, update, and customize handbooks that fit your organization with one simple tool.
Job Description Manager
Over 2,000 job descriptions are ready for your customization, complete with team-based approvals.
Job Classification & FLSA Audit
Gain peace of mind that your FLSA practices are in compliance with automated risk assessments.
Salary Finder
Ensures instant access to the salary data you need to make smart and competitive pay decisions.
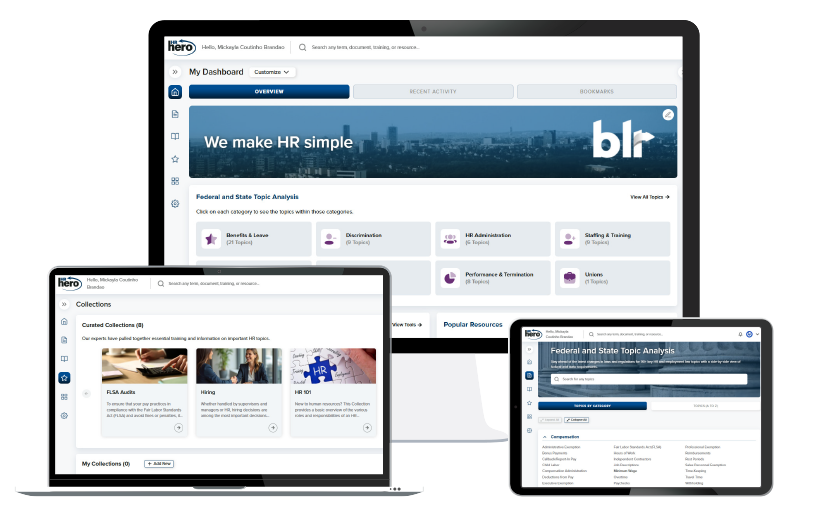
Federal and State Topic Analysis
A side-by-side, deep dive into 90+ key employment laws and requirements.
HR Hotline
Get the answers you need when you need them. Clear, and concise answers to your most pressing questions.
The how-to behind your HR strategy
Our platform is designed to streamline HR processes, saving valuable time and allowing HR teams to focus on strategic initiatives. HR Hero provides practical solutions that address real-world HR challenges, offering step-by-step guidance and actionable recommendations based on industry best practices and legal compliance requirements.
415 hrs
time saved annually streamlining critical tasks
4.3
average client score from Capterra and G2
5.7x
average number of times HR Hero subscribers have renewed
75%
of clients use HR Hero every week
“The analysis between both federal and state law, that is the one thing that I have not found anywhere else, that is the most helpful to me, especially when I am updating a policy.“
SHARETA, VICE PRESIDENT OF HR AT VA DESERT PACIFIC FEDERAL CREDIT UNION
Case studyExcellence
We bring a collective 100+ years of industry expertise. Leverage our expertise to unlock your team’s potential






